Hip and Knee Joint Replacement – Is Same Day Discharge Possible?
Aug 22, 2019Joint replacement surgeries have evolved over the past several decades with focus on safety, accuracy, reproducibility and rapid recovery. Outpatient surgery has become a reality in most surgical faculties. Hip and knee replacement is one of the most commonly performed surgeries in adult orthopedics. The procedure was once considered one of the most painful orthopaedic surgeries. The average length of stay for these procedures has come down to 3 days from a traditional 10 days in the past. The major deterrent for early discharge was the postoperative? pain control. With the advent of multimodal analgesia, which has proven to have an Opioid-sparing effect, outpatient joint replacement has become a reality for the motivated patient.
The trend for outpatient hip and knee replacements has been progressively increasing over the last few years globally. This has been dictated mostly due to the well-informed patient who is interested in the procedure and outcome, and to a certain extent the economics involved. Individual surgeons, hospitals and insurance companies have shown interest after careful consideration of the safety and cost benefit for the society. The advancements in blood loss, minimally invasive surgery, and rapid recovery protocols with physical therapy have made the dream come true for the joint surgeon. The important factors which can favor this procedure include preoperative screening of the patient’s medical co morbidities and home environment.
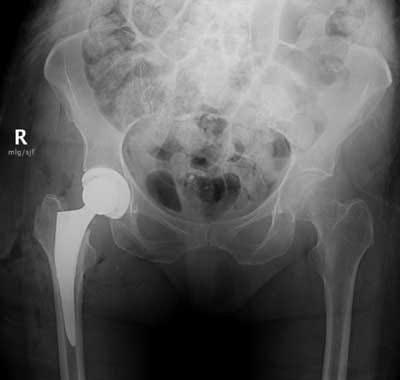
PREOPERATIVE PATIENT INFORMATION- PREPARING FOR OUTPATIENT JOINT REPLACEMENT SURGERY
The major complications following a hip and knee replacement surgery include but are not limited to infection, deep vein thrombosis (DVT), pulmonary embolism, dislocation of the joint, stiffness, persistent pain, leg length discrepancy, and blood transfusions. The Surgical Care Improvement Project (SCIP) protocols initiated by the Joint commission have made a tremendous impact on the use of proper antibiotic prophylaxis to prevent infection and DVT. Early mobilization, portable DVT prevention therapy systems and thermal compression therapy have helped with pain control, DVT prophylaxis and rapid recovery.
Careful selection of patients for outpatient arthroplasty is imperative for the safety and successful outcomes. The patients are leaving the hospital before pain breakthrough and likely complications from co morbidities. Preoperative screening is very important. Patients with cardiac disease (congestive heart failure, atrial fibrillation, recent myocardial infarction,), pulmonary abnormality (COPD, sleep apnea, emphysema, pulmonary hypertension), cirrhosis, uncontrolled diabetes, history of DVT and genitourinary disease have a high prevalence for readmission. Also patients with elevated body mass index and advanced age carry a slightly higher risk for these procedures as outpatient. Coming to the office visit prepared with a complete medical history will help your surgeon to assess your risk comprehensively.
- Surgeons and hospitals prefer that the patients undergo the surgical procedure early in the day to give adequate time for the physical therapist to fulfill functional discharge criteria.
- It is mandatory to have a caregiver at home for the first 24-48 hours.
- The ability to reach a staff member for advice on pain breakthrough, wound drainage, dizziness, nausea, constipation is crucial.
The expectations of the patient and the patient’s family and the ability of the surgeon and his healthcare team must be in alignment.
PRE ANESTHETIC TESTING (PAT) AND JOINT CLASS
Healthcare institutions, which have Joint Commission accreditation focus on adequate testing of the patient prior to surgery. This will be coordinated by your surgeon’s office, your family physician and your hospital where you are likely to undergo surgery. It is well known that preoperative indication reduces patient anxiety, decreases pain and increase overall satisfaction. Your family physician can assess your overall risk and provide valuable information and input to your surgeon. If you have any medical co morbidities, it is imperative to have a medical clearance.
The requirements for physical therapy and rehabilitation must be arranged including provision of crutches, practicing walking with them, stair training, elevated toilet seat, grabber, shoe kit etc. Home health for physical therapy should be arranged the evening or the next day after the surgical procedure.
Please call and verify with your insurance provider whether your surgeon and the hospital are in the network. Obtain information regarding your benefits for home health and outpatient physical therapy.
PERIOPERATIVE PAIN MANAGEMENT
Modern perioperative pain management includes multimodal and preventive analgesia. The term multimodal means the combination of more than one class of analgesic drugs, improves pain control and has the ability to minimize opioids. Preventive analgesia extends to the preoperative and post-discharge pain control measures. A dedicated and enthusiastic orthopedic anesthesia team is an integral part of outpatient joint replacement surgery. Short-acting spinal and analgesic with or without adductor canal block and sciatic nerve block will minimize the necessity for narcotics during surgery. This, in turn will decrease the nausea and blood pressure variations postoperatively.
BLOOD LOSS MANAGEMENT
Hip and knee replacements have traditionally been associated with substantial blood loss during and after the surgery. The importance of improving hemoglobin prior to this elective procedure cannot be emphasized enough. Use of certain medications like tranexamic acid have drastically decreased the intra-and postoperative blood loss.
HEALTH CARE TEAM FOR A SAFE PROCEDURE, SATISFACTORY EXPEREIENCE & SUCCESSFUL OUTCOME
The pivotal role is played by your surgeon and hospital with adequate surgical volume, and experience to improve your outcome. Your surgeon’s front desk, medical assistant, medical records and financial counselor help in various aspects of your surgery. The surgical team including the anesthesiologist, the nursing staff, scrub tech, your surgeon’s first assist, and the implant vendor help in performing the procedure safely and efficiently. Recovery is heavily dependent on your physical therapist and your compliance with the therapy.
WHEN NOT TO CONSIDER OUTPATIENT JOINT REPLACEMENT
Patients with opioid dependence, smoking, above ideal weight, cardiac conditions, pulmonary conditions, uncontrolled diabetes, chronic medical conditions, psychiatric disturbances are in general a contraindication for outpatient hip and knee replacements.
In summary, outpatient joint replacements for hip and knee arthritis can be performed safely. The emphasis has been on the patient experience. The expectations of the patient and the patient’s family and the ability of the surgeon and his healthcare team must be in alignment.
Minimally invasive surgery, material advancements, and precision in placement of implants have given confidence to release patients home same day after joint replacement surgery.



 Our patients can receive MRI imaging onsite at both our Louisville and New Albany Clinics.
Our patients can receive MRI imaging onsite at both our Louisville and New Albany Clinics. Providing the latest advances in orthopedic surgery is our specialty.
Providing the latest advances in orthopedic surgery is our specialty. We take a unique, multidisciplinary approach to pain management.
We take a unique, multidisciplinary approach to pain management. Our physical therapists use advanced techniques to help restore strength and mobility.
Our physical therapists use advanced techniques to help restore strength and mobility.  We provide comprehensive, conservative care for a wide variety of foot and ankle conditions.
We provide comprehensive, conservative care for a wide variety of foot and ankle conditions. We offer same- and next-day care to patients with acute injuries.
We offer same- and next-day care to patients with acute injuries. Get back in the game with help from our sports medicine specialists.
Get back in the game with help from our sports medicine specialists.  Our centers are equipped with a state-of-the-art digital X-ray machine.
Our centers are equipped with a state-of-the-art digital X-ray machine.