Controversies in Foot and Ankle Trauma: Fractures of the Proximal Fifth Metatarsal
Aug 21, 2019George Edward Quill, M.D. (Retired 2023)
Introduction
Most of the controversy regarding fractures of the fifth metatarsal relates to those injuries sustained in the proximal one-third of the bone. Controversies in diagnosing and classifying fractures of the proximal one-third of the fifth metatarsal are common, and have been perpetuated by a rather lax usage of anatomic terms and applications of eponyms such as the Jones fracture.1,2,6,8,9,13,18,28 With regard to fractures of the proximal diaphysis of the fifth metatarsal, controversies exist regarding the importance of the acuity or chronicity of prodromal symptoms, the incidence and potential cause of delayed unions and nonunions of this portion of the bone, as well as determining the most optimal method of treatment.1-5,7,9-11,19,20,22
The orthopaedic literature is replete with articles distinguishing between fractures of the tuberosity of the fifth metatarsal, those of the metaphysis, and those at the metaphyseal-diaphyseal junction.1-11,13-20,22,23 Controversy regarding treatment of fractures in this area centers around whether the treatment should be closed or open, primary or delayed, whether the fracture should be bone grafted or fixed with an intramedullary screw or other internal fixation device, and whether the athlete should be treated any differently initially than the more sedentary person sustaining the same fracture. There also is debate regarding the rate of reinjury of the proximal one-third of the fifth metatarsal.
This chapter will serve as an overview of proximal fifth metatarsal fractures, covering the etiology, mechanisms of injury, and the pertinent anatomy of this injury. We will propose a classification scheme for fractures of the fifth metatarsal and give some historical – as well as practical – detail with regard to the treatment of each fracture type. A series of fifth metatarsal fractures and treatment with results and followup examination will be presented. A practical treatment algorithm for fractures of the fifth metatarsal is offered to hopefully minimize future misunderstanding with regard to patient treatment.
Fractures of the Proximal Fifth Metatarsal
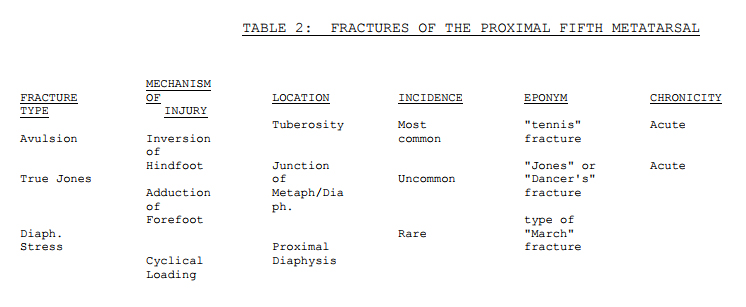
There are at least three, and probably six fracture types, that occur with any degree of frequency in the proximal fifth metatarsal.9,19We will consider the fifth metatarsal tuberosity avulsion fracture (Figure 1a), the (acute) Jones fracture (Figure 1b), and the proximal diaphyseal stress fracture (Figure 1c), which has been described as having three subtypes (See Table 1).19,20,22 Also occurring in this area in the immature foot are apophyseal distraction types of fifth metatarsal fractures. These injuries must be distinguished from injury to the sesamoid (os peroneum, os vesalianum) and tarsometatarsal complex, which can also commonly cause pain in the dorsolateral, proximal forefoot.
As varied as these fractures are, most fifth metatarsal fractures heal with immobilization. Surgical treatment may be required for certain proximal fifth metatarsal fractures to speed recovery time or to salvage delayed unions or nonunions. Surgery may also be indicated for displaced or intra-articular fractures.
Anatomy of the fifth metatarsal: The fifth metatarsal consists of a head, neck, shaft, tuberosity, and base (Figure 2).9 The tuberosity has also been referred to as the styloid process of the metatarsal. At its proximal end, the fifth metatarsal articulates at the cuboid-fourth metatarsal joint, the cuboid-fifth metatarsal joint, and the 4-5 intermetatarsal joint. Although there are individual anatomic variations, the tuberosity usually protrudes downward and laterally beyond the margin of the diaphysis and the adjacent cuboid. The peroneus brevis inserts over a relatively large area on the dorsolateral aspect of the tuberosity. The peroneus tertius tendon inserts more on the lateral surface of the metatarsal diaphysis distal to the tuberosity. The abductor digiti minimi has its origin on the lateral and medial processes of the os calcis, calcaneal fascia, and the adjacent intermuscular septum. This muscle passes under and around the base of the fifth metatarsal with a variable attachment to the bone. The muscle then continues distally to insert into the lateral side of the base of the proximal phalanx of the little toe.21 Dameron reports that this midportion attachment of the abductor digiti minimi was present in 18 of 20 feet he dissected.4 In his anatomical series, only the peroneus brevis tendon appeared to be sufficiently strong in its attachment to the base of the fifth metatarsal in these 20 feet to cause avulsion of a bone fragment with inversion or adduction forefoot injury.
The flexor digiti minimi brevis has its origin on the base of the fifth metatarsal, while the dorsal and plantar interossei originate on the shaft of this bone.4,21
In 1984, Richli and Rosenthal attributed the commonly seen transverse fracture through the base of the fifth metatarsal to avulsion by the lateral cord of the plantar aponeurosis.16 Although these authors could not produce a fracture by stressing the cadaver foot with the peroneus brevis intact, they felt that the tuberosity avulsion fracture caused by inversion and plantar flexion of the forefoot is due to traction on the lateral cord of the plantar fascia, and is not due to avulsion at the peroneus brevis insertion in the in vitro setting. These authors, as well as others, are quick to differentiate this injury from the true Jones fracture or proximal diaphyseal stress fractures, and concluded that the avulsion fracture is a relatively benign fracture that heals well with conservative treatment. Many authors do not agree that the etiology of this injury is related to the plantar aponeurosis, and recognize the importance of the attachment of the peroneus brevis.
Sir Robert Jones felt that the cuboid-4,5 metatarsal articulation was so secured by ligamentous attachments and joint capsule, as well as by the plantar fascia and broad insertion at the peroneus brevis, that injury here resulted in fracture of the fifth metatarsal rather than at the tarsometatarsal joint.13 The true Jones fracture probably occurs with the ankle plantar flexed, when a significant adduction force is applied to the forefoot.
A secondary ossification center within the proximal end of the fifth metatarsal is not commonly present before age 8 years in either sex. This apophysis runs parallel to the shaft along the lateral inferior margin of the tubercle of the fifth metatarsal on x-ray. Fractures in this area usually occur perpendicular to the long axis of the shaft. This apophyseal center does not extend proximal to the tarsometatarsal or 4, 5 intermetatarsal joints as a fracture often does. This small area of mineralization is usually radiographically visible between the ages of 9 and 11 years in girls and between 11 and 14 years in boys.4 It is usually less than 2 years between the appearance of this apophysis and its radiographic union to the shaft.
With the foregoing age ranges in mind, Dameron has noted that this apophysis may commonly be absent in children in this age group. Up to 50 percent of the children in this age range followed chronologically by Dameron did not have this apophysis demonstrated radiographically.4
Dameron has reported the os peroneum to be present within the peroneus longus tendon, near the proximal portion of the fifth metatarsal, but adjacent to the cuboid, in 15 percent of unselected foot radiographs (Figure 3). In the same series, he identified an os vesalianum in 0.1% of these feet. When it was identified, the os vesalianum was more irregularly shaped, longitudinally oriented, and found proximal to the insertion of the peroneus brevis on the proximal tip of the fifth metatarsal.4
Classifications of proximal fifth metatarsal fractures: I am proposing the classification scheme outlined in Table I to aid in the management of proximal fifth metatarsal fractures. I have found this classification to be practical and to aid in assisting the individualization of patient treatment. This fracture scheme should also provide for better communication between treating surgeons and in published descriptions of this injury. Imprecise use of the term Jones fracture and failure to distinguish the true acute Jones fracture from stress fracture of the proximal diaphysis, as well as from tuberosity avulsion fractures has created confusion in our literature (Figure 4).
Tuberosity avulsion fractures: The most common fracture of the proximal fifth metatarsal is the tuberosity avulsion fracture.9 Past authors have attributed this fracture to tuberosity avulsion by the contracting peroneus brevis muscle when the hindfoot is inverted. Cadaveric studies would lead us to believe that it is the firm attachment of the lateral band of the plantar aponeurosis that is the structure more likely causing tuberosity avulsion fractures than is the peroneus brevis. Most of these fractures occur at the tip of the tuberosity where the plantar aponeurosis attaches, the peroneus brevis inserting more distal than this.14,16 Only rarely is fracture displacement seen, even when the fracture is not immobilized (Figure 1a). Certainly, were the peroneus brevis the cause of the avulsion, muscular contraction and spasm would cause some displacement in the patient who was not immobilized.
This common tuberosity avulsion fracture is usually extra-articular, and it is occasionally associated with a concomitant lateral malleolus fracture that must not be overlooked by the treating physician.12 When larger pieces of bone are avulsed, the fracture line may extend into the cuboid-metatarsal joint, and displacement of this intra-articular fracture may necessitate operative fixation. If operative treatment is selected, many options for fixation are available, but, if comminuted, it is often simpler to excise the fracture and re-attach the insertion of the peroneus brevis to the metatarsal.
It is appropriate to mention again here two types of injury commonly mistaken for tuberosity avulsion fractures.
Girls between the ages of 9 and 11 years and boys between 11 and 14 years old who commonly sustain inversion injuries of the foot and ankle may, have a tuberosity apophysis present on x-ray without fracture and have a good prognosis with closed management. The nondisplaced tuberosity avulsion fracture will not have the smooth radiolocent line parallel to the metatarsal shaft that the apophysis has, and the fracture line is commonly perpendicular to the shaft of the bone. The tuberosity apophysis usually unites with the rest of the bone two to three years after its occurrence, and almost no adolescent of either sex older than 16 years still has an ununited apophysis present.
The os peroneum is often seen adjacent to the lateral border of the cuboid within the peroneus longus tendon. The painful os vesalianum is found adjacent to the peroneus brevis insertion and has smooth edges unless the ossicle itself is fractured.
The recommended treatment of tuberosity avulsion fractures is generally “symptomatic care”.8,9,12 A compressive wrap or ambulating to tolerance in a hard-soled shoe have been espoused as the treatment of choice. However, pain is a highly subjective complaint, and pain tolerance varies greatly from patient to patient. I have found that the patient with a nondisplaced, extra-articular tuberosity avulsion fracture will be most comfortable when treated with protected weight bearing to tolerance in some type of fracture orthosis or cast that immobilizes both the foot and the ankle. This device may be discarded within three to six weeks as symptoms allow.
The displaced or intra-articular tuberosity avulsion fracture with excessive articular step-off is treated with open reduction, internal fixation using mini-fragment plates and screws, closed reduction and pinning, or tension band wiring. A utilitarian approach to this and other fractures of the proximal fifth metatarsal is closed, intra-medullary cannulated screw fixation. This technique will be discussed below.
The Jones fracture of the proximal fifth metatarsal: The true Jones fracture is an acute forefoot injury that occurs with no prodrome or preponderance for age, sex, occupation, or sport (Figure 1b).9 Stewart defined the true Jones fracture as a transverse fracture at the junction of the diaphysis and metaphysis, without extension distal to the 4,5 intermetatarsal articulation.18 Medial comminution commonly is present. This fracture may be considered intra-articular and to be involving the fourth and fifth intermetatarsal articular facet, but should not be diagnosed if the main fracture line extends into the metatarsocuboid joint.
Unlike the proverbial lawyer who defends himself in court and has a fool for a client, Sir Robert Jones diagnosed his own injury and described the ultimate doctor-patient relationship as follows:
“Some months ago, whilst dancing, I trod on the outer side of my foot, my heel being off the ground. Something gave way midway down my foot, and I at once suspected a rupture of the peroneus longus tendon. By the help of a friend, I managed to walk to my cab, a distance of over 300 or 400 yards. The following morning I carefully examined my foot and discovered that my tendon was intact. There was a slight swelling over the base of the fifth metatarsal bone. I endeavored to obtain crepitus and failed. A finger on the spot gave exquisite pain. Body pressure on the toes, even the slightest, was painful; but when the pressure was deviated to the outer side, the pain was still greater. Extension of the ankle and flexion of the toes were immediately felt at the base of the fifth metatarsal.
I hobbled down stairs to my colleague, Dr. David Morgan, and asked him to x-ray my foot. This was done, and the fifth metatarsal was found to be fractured about three-fourths of an inch from its base.”13
In a 1902 edition of the Annals of Surgery, Jones’ report of 6 patients with fractures of the proximal portion of the fifth metatarsal was one of the first applications of diagnostic radiography published. The first patient in his series was himself. Perhaps some of the controversy over what constitutes a true Jones fracture stems from the fact that the reproduction of Jones’ original foot x-ray is not readily interpreted. The films of other patients in his report, however, fit the description of the fracture described by Stewart above. It would seem that an adductor moment across the relatively fixed fourth and fifth metatarsal bases causes an acute fracture of the base of the fifth metatarsal at the area between the insertion of the peroneus brevis and tertius tendons. Even though the fourth and fifth metatarsals have good range of motion in the parasagittal plane, they are relatively immobile in the transverse plane, and this area of the foot serves as a fulcrum over which the fracture is sustained with adduction of the forefoot.
Many series, including Stewart’s published in 1960, claim the frequent occurrence of delayed union or nonunion is associated with nonoperative management of proximal fifth metatarsal fractures. It is quite likely that a good number of the fractures classified as “Jones fractures” in Stewart’s and other authors’articles were actually diaphyseal stress fractures, which had a much poorer likelihood of healing with nonoperative management than did the acute, true Jones fracture. In 1972 Dameron reported on 20 patients with fractures “within the proximal 1_ centimeters” of the metatarsal shaft.4 Most of these were indeed diaphyseal stress fractures, but some were probably Jones fractures. Seventy percent of his patients were less than 21 years of age. After 8 weeks of treatment, 5 out of 5 of the fractures treated with bone graft healed, 12 of 15 healed with further immobilization (up to 12 months) and 3 out of 15 healed with nonoperative management, but took up to 21 months to do so. Dameron (1972) and Kavanaugh (1978) reported a high re-fracture rate with nonoperative care for proximal fifth metatarsal fractures.4,8
If one is to interpret these last several articles at face value, it would appear that the vast majority of “Jones fractures”, that is, about 75 percent, will heal if casted for a long enough period of time. However, 1/3 of these injuries managed closed will re-fracture if followed long enough. Twenty-five percent of all patients with proximal fifth metatarsal fractures that were not tuberosity avulsion fractures will statistically not heal with closed management no matter how long they are followed. Of those 75 percent that do heal, according to the current literature, 1/3 of them will re-fracture with nonoperative treatment. It follows that one could make an argument for early operative management, either with medullary screw fixation or bone grafting, since 50 percent (1/4 plus 1/3 of 3/4) of fractures treated closed will either not heal primarily, or will re-fracture once initial healing has been documented.
For the purposes of this chapter, and so that there will be less misunderstanding in future reports, I would like to adhere to the classification of these fractures given in Table 1. We, therefore, will classify Jones fractures as an acute injury and recommend the following treatment.
The acute, nondisplaced Jones fracture should be treated with nonweight bearing ambulation in a short leg cast for 6 to 8 weeks, except in the high performance athlete or the informed patient who is not at all interested in conservative care. I personally prefer to operate these patients early on with medullary cannulated screw fixation. For the professional athlete, a decision for operative versus nonoperative care may be influenced by the chronologic proximity to the playing season.
If the physician treating a patient with an acute, nondisplaced true Jones fracture elects for conservative care and sees no radiographic evidence for healing at 6 to 8 weeks, then the treatment should be individualized according to patient needs and expectations. Intramedullary sclerosis and a lucent fracture line are relative indications for surgery. Continued protection, maybe even in a removable fracture orthosis, may be considered prudent. One could also make an argument for operating with medullary screw fixation or bone grafting the patient with an acute nondisplaced proximal fifth metatarsal Jones fracture that does not demonstrate adequate healing at 6 to 8 weeks.
The patient with the acute Jones fracture that is displaced, should undergo early operative fixation with either closed medullary cannulated screw fixation or the surgeon’s preference from the following: tension band wiring, mini-fragment screws and plates that are low profile, or cross-pinning with K-wires with further immobilization. The advantages of closed medullary screw fixation employing a cannulated screw technique with intraoperative fluoroscopic guidance are that the technique is relatively technically uninvolved, the technique does not open the fracture site, and if the screw is placed appropriately, there is no need for subsequent hardware removal (Figure 5). There is some controversy regarding hardware removal in high-performance basketball players, particularly who have a cavus foot shape. Screw removal in these patients is associated with an increased incidence of re-fracture.
Employing this technique, I position the patient in the semi-lateral decubitus position and use intraoperative C-arm fluoroscopy. A tourniquet may or may not be necessary. A 3 centimeter incision paralleling the plantar border of the foot without invading the plantar pad is made beginning at the level of the tuberosity, extending proximally. The wound needs to extend proximally far enough so that one can medialize the proximal end of the cannulated guide wire. With the patient in this position and the foot resting in the plane of a 30 degree internal oblique fluoroscopic beam, the guide wire may be inserted down the medullary shaft parallel to the plantar border of the foot. The guide wire should engage cortex near the neck of the fifth metatarsal distally, but not violate that cortex. A direct measurement of the screw length, allowing for countersinking of the head should be made. I use a 7 millimeter cannulated screw (Synthes, Paoli, Pennsylvania). I usually choose a screw between 40 and 55 millimeters long. The screw length depends upon the length of the metatarsal and the diameter of the narrowed portion of the diaphysis (isthmus). If the isthmus is narrow, a 4.5 millimeter cannulated screw may be sufficient for fixation.
I prefer the screw that has no more than a 16 millimeter thread length so that all the threads can gain purchase distal to the fracture site for compression. The cannulated screw is passed over the guide wire, x-rays are obtained, and the wire is removed. The patient is then immobilized in a plaster splint, which may be changed to a weight bearing short leg cast at two weeks’ time when sutures are removed. In our series, one nonunion occurred with this technique in a patient who most likely had a pathologic fracture through dysplastic bone to begin with.
Proximal fifth metatarsal diaphyseal stress fractures: Neither the history nor the biologic behavior of this type of fifth metatarsal fracture seems to parallel comparable fractures of other metatarsals. The treating physician needs to address the needs and expectations of the patient. This fracture behaves quite differently from the tuberosity avulsion fracture and the true, acute Jones fracture. This is a fracture resulting from repetitive cyclical forces applied to the foot (Figure 1c). Devas has defined the stress fracture as a spontaneous fracture of normal bone which results from the summation of stresses, any of which by themselves would be harmless.5 Thus this type of diaphyseal stress fracture is associated with prodromal symptoms that may result in an acute-on-chronic episode before the patient presents. The surgeon looks for reparative responses in the bone, such as cortical stress hypertrophy and narrowing of the medullary canal and periosteal reaction. This type of fracture is definitely more rare than the other subtypes which are sustained acutely
In 1978 Kavanaugh reported that 41 percent of the patients in their series with fractures of the fifth metatarsal had prodromal symptoms.8 In 1979 Zelko and Torg identified in 14 of their 21 patients (67 percent) a lucent fracture line with periosteal reaction at the initial presentation.22
In 1983 DeLee reported a series of athletes who all had a history of prodromal symptoms over the lateral aspect of the foot prior to the acute episode which precipitated presentation to the orthopaedist, roentgenographic evidence of stress phenomenon in all of the fifth metatarsals in the series, and no history of previous treatment for fifth metatarsal fractures.5 Union was obtained in all 10 athletes who met these criteria for stress fracture at an average of 7_ weeks after early axial intramedullary screw fixation. Seven of the 10 patients in that series, however, complained of local pain over the screw head. The reader is referred to DeLee’s article for clarification of his technique for screw fixation.
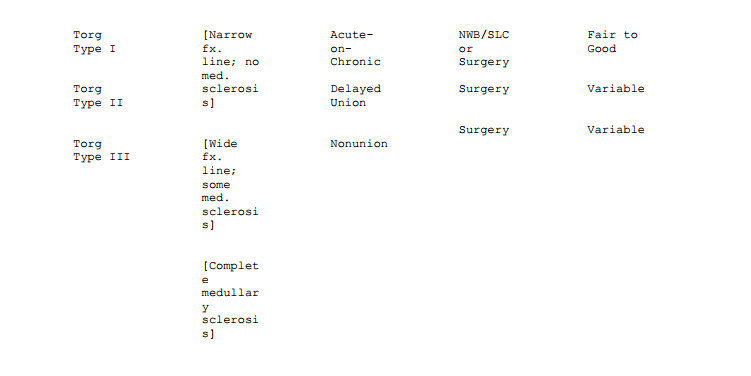
In 1984 Torg published an article which really helps to distinguish the healing potential of fifth metatarsal diaphyseal fractures.20 In this report he subclassified diaphyseal stress fractures of the fifth metatarsal into those that were acute (or early), delayed, and nonunions.
What he called an acute fracture was an early diaphyseal stress fracture with periosteal reaction which represents an attempt of the bone to heal an incomplete fracture. The fracture type he called delayed union had evidence for a lucent fracture line and medullary sclerosis. The obvious, established nonunions had complete medullary obliteration. These three subtypes of fifth metatarsal stress fracture are though to represent a radiographic continuum of the typical stress fracture.
We have treated the (Torg) Type I diaphyseal stress fractures in the same manner as acute, nondisplaced Jones fractures. Treatment may be prolonged nonweight bearing and immobilization or, in the appropriately selected patient, early operative fixation. The Type II diaphyseal stress fracture should be treated operatively with bone graft or medullary screw fixation, especially in the competitive, vigorous, or heavyset patient. A much less vigorous patient could perhaps still be managed with prolonged nonweight bearing immobilization.
The patient with a Type III diaphyseal fifth metatarsal stress fracture has a symptomatic nonunion and will require surgical intervention. I prefer closed, cannulated medullary screw fixation over open methods, including tricortical inlay bone graft. Employing this algorithmic approach to proximal fifth metatarsal fracture management, this author has achieved a 100 percent union rate for tuberosity avulsion fractures of the fifth metatarsal, acute Jones fractures, and for Torg Subtype I and II diaphyseal stress fractures of the fifth metatarsal. Our only nonunion in a series of 35 consecutive proximal fifth metatarsal fractures treated over the last 4 years was encountered in a patient with a Torg Subtype III established nonunion of a diaphyseal stress fracture. Even at cessation of treatment this patient was asymptomatic. Her case is an unusual one in that she had dysplastic bone that most likely represented a case of osteogenesis imperfecta. At release from active orthopaedic treatment, she had an asymptomatic fibrous type of union of her diaphyseal fifth metatarsal stress fracture.
Employing this treatment protocol, the 35 fractures treated in this series were broken down as follows. The 14 tuberosity avulsion type fractures were sustained in patients who had an average age of 29_ years and had an average time to union of 6.1 weeks. All of these were treated closed. The 12 patients treated for Jones fractures had an average age of presentation of 41 years and healed with treatment dictated by this protocol at an average of 7.4 weeks. All but one of these patients was treated with an intramedullary large fragment screw. Of the 9 patients presenting with a diaphyseal stress fracture, they healed at an average of 6_ weeks and had a mean age of presentation of 37 years. All of these patients were treated operatively with our closed medullary screw fixation technique.
Current orthopaedic literature does not contain a published report in which electrical stimulation has been evaluated by a prospective, randomized treatment protocol. Even though his study is not randomized and not prospective, Holmes is reporting data in which he treated delayed union and nonunion of the proximal fifth metatarsal with pulsed electromagnetic fields.7 All 9 of the fractures in this series healed in a mean time of 4 months with a range of 2 to 8 months. Those fractures treated with both pulsed electromagnetic fields and a nonweight bearing cast for the entire time of the study healed in a mean time of three months with a range of 2 to 4 months. Holmes refers to these injured feet as having Jones fractures with clinical and radiographic signs of delayed union and nonunion. It is apparent to me upon review of this series, however, that this series includes both true Jones fractures and diaphyseal stress type fractures of the proximal 1/3 of the fifth metatarsal.
Table 2 is presented to summarize fifth metatarsal fracture characteristics and recommended treatment. In summary, further controversy and misunderstanding regarding proximal fifth metatarsal fractures may be minimized if one considers the classification scheme detailed in this chapter. Tuberosity avulsion fractures are acute injuries, the majority of which can be treated closed. Operative intervention for these injuries is indicated if the fracture fragment is either very large and associated with a good deal of morbidity, or intra-articular and significantly displaced.
The Type II proximal fifth metatarsal fracture, otherwise known as the true acute Jones fracture, may be treated with nonweight bearing short leg cast immobilization, except in the vigorous or athletic patient, who should probably undergo early closed medullary screw fixation. The acute Jones fracture that is displaced on initial presentation should also undergo early operative intervention.
Treatment for the Type I diaphyseal stress fracture parallels that for the acute nondisplaced Jones fracture. The Type II diaphyseal stress fracture should be bone grafted or undergo medullary screw fixation, especially in the competitive athlete or vigorous patient. The Type III diaphyseal stress fracture represents a symptomatic, established nonunion and will require surgical intervention in the form of bone grafting and/or screw fixation.
References
- Acker JH, and Drez, Jr., D: Nonoperative Treatment of Stress Fractures of the Proximal Shaft of the Fifth Metatarsal (Jones Fracture), Foot and Ankle, Vol. 7, No. 3:152-155, 1986.
- Arangio GA: Proximal Diaphyseal Fractures of the Fifth Metatarsal (Jones Fracture): Two Cases Treated by Cross-Pinning with Review of 106 Cases, Foot and Ankle, Vol. 3, No. 5:293-296, 1983.
- Carp L: Fracture of the Fifth Metatarsal Bone with Special Reference to Delayed Union, read before the Orthopaedic Section of the New York Academy of Medicine, April 15, 1927.
- Dameron TB: Fractures and Anatomical Variations of the Proximal Portion of the Fifth Metatarsal, Journal of Bone and Joint Surg., 57A:788-792, 1972.
- DeLee JC, Evans JP, and Julian J: Stress Fracture of the Fifth Metatarsal, The American Journal of Sports Medicine, Vol. 11, No. 5: 349-353, 1983.
- Hens J, and Martens M: Surgical Treatment of Jones Fractures, Archives Orthopaedic Trauma Surgery, 109:277-279, 1990.
- Holmes, Jr., GB: The Treatment of Delayed Unions and Nonunions of the Proximal Fifth Metatarsal with Pulsed Electromagnetic Fields, unpublished data, 1994, personal communication.
- Kavanaugh JH, Brower TD, and Mann RV: The Jones Fracture Revisited, Journal of Bone and Joint Surg, 60A:776-782, 1978.
- Lawrence SJ, and Botte MJ: Jones Fractures and Related Fractures of the Proximal Fifth Metatarsal, Foot and Ankle, Vol. 14, No. 6:358-365, 1993.
- Lehman RC, Torg JS, Pavlov H, and DeLee JC: Fractures of the Base of the Fifth Metatarsal Distal to the Tuberosity: A Review, Foot and Ankle, Vol. 7, No. 4:245-252, 1987.
- Lichtblau S: Painful Nonunion of a Fracture of the Fifth Metatarsal, Clinical Orthopaedics, Vol. 59:171-175, 1968.
- Pearson JR: Combined Fracture of the Base of the Fifth Metatarsal and the Lateral Malleolus, Journal of Bone and Joint Surg., Vol. 43A, No. 4: 513-516, 1961.
- Peltier LF: Eponymic Fractures: Robert Jones and Jones’ Fracture, Surgery Vol. 71, No. 4:522- 526, 1972.
- Pritsch M, Heim M, Tauber H, and Horoszowski H: An Unusual Fracture of the Base of the Fifth Metatarsal Bone, The Journal of Trauma, Vol. 20, No. 6:530-531, 1980.
- Rettig AC, Shelbourne KD, and Wilckens J: The Surgical Treatment of Symptomatic Nonunions of the Proximal (Metaphyseal) Fifth Metatarsal in Athletes, The American Journal of Sports Medicine, Vol. 20, No. 1:50-54, 1992.
- Richli WR, and Rosenthal DI: Avulsion Fracture of the Fifth Metatarsal: Experimental Study of Pathomechanics, AJR Vol. 145:889-891, 1984.
- Smith JW, Arnoczky SP, and Hersh A: The Intraosseous Blood Supply of the Fifth Metatarsal: Implications for Proximal Fracture Healing, Foot and Ankle, Vol. 13, No. 3:143-152, 1992.
- Stewart IM: Jones’ Fracture: Fracture of Base of Fifth Metatarsal, Clinical Orthopaedics, Vol. 16:190-198, 1960.
- Torg JS: Fractures of the Base of the Fifth Metatarsal Distal to the Tuberosity: A Review, Contemporary Orthopaedics, Vol. 19, No. 5:497-505, 1989.
- Torg JS, Balduini FC, Zelko RR, Pavlov H, Peff TC, and Das M: Fractures of the Base of the Fifth Metatarsal Distal to the Tuberosity, Journal of Bone and Joint Surg., 66A:209-214, 1984.
- Warfel JH, The Extremities, Fourth Edition, Lea and Febiger, Philadelphia, 1974.
- Zelko RR, Torg JS, and Rachun A: Proximal Diaphyseal Fractures of the Fifth Metatarsal – Treatment of the Fractures and Their Complications in Athletes, American Journal of Sports Medicine, Vol. 7, No. 2:95-101, 1979.
- Zogby RG, and Baker BE: A Review of Nonoperative Treatment of Jones Fracture, The American Journal of Sports Medicine, Vol. 15, No. 4:304-307, 1987.

Lengends for Figures
Figure 1a: Oblique radiograph of fifth metatarsal tuberosity avulsion fracture.
Figure 1b: Oblique radiograph of a Jones fracture.
Figure 1c: Oblique radiograph of a fifth metatarsal proximal diaphyseal stress fracture.
Figure 2: Schematic anatomy of the fifth metatarsal (after Lawrence and Botte, Foot and Ankle, Volume 14, No. 6, 1993; used with permission). H = Head, N = Neck , S = Shaft , B = Base , T = T 21 uberosity,PT = Peroneus Tertius, PB = Perone 22 us Brevis, PF = Lateral Bandof Plantar 23 Aponeurosis/Fascia
Figure 3: The os peroneum lies within the peroneus longus tendon adjacent to the border of the cuboid.
Figure 4: Schematic illustration of fracture zones for proximal fifth metatarsal fractures (from Lawrence and Botte, “Foot Fellow’s Review: Jones’Fracture and Related Fractures of the Proximal Fifth Metatarsal”, Foot and Ankle, Volume 14, No. 6, 1993; used with permission).
Figure 5: Oblique radiograph of a proximal fifth metatarsal fracture treated with medullary cannulated screw fixation.
Mark S. Myerson, Editor



 Our patients can receive MRI imaging onsite at both our Louisville and New Albany Clinics.
Our patients can receive MRI imaging onsite at both our Louisville and New Albany Clinics. Providing the latest advances in orthopedic surgery is our specialty.
Providing the latest advances in orthopedic surgery is our specialty. We take a unique, multidisciplinary approach to pain management.
We take a unique, multidisciplinary approach to pain management. Our physical therapists use advanced techniques to help restore strength and mobility.
Our physical therapists use advanced techniques to help restore strength and mobility.  We provide comprehensive, conservative care for a wide variety of foot and ankle conditions.
We provide comprehensive, conservative care for a wide variety of foot and ankle conditions. We offer same- and next-day care to patients with acute injuries.
We offer same- and next-day care to patients with acute injuries. Get back in the game with help from our sports medicine specialists.
Get back in the game with help from our sports medicine specialists.  Our centers are equipped with a state-of-the-art digital X-ray machine.
Our centers are equipped with a state-of-the-art digital X-ray machine.