The Quest for the Perfect Knee Replacement
Aug 22, 2019Richard A. Sweet, M.D. (Retired 2022)
Introduction:
General Concepts
Total knee replacement surgery has become a highly successful operative procedure. Recent advances in minimally invasive techniques have shortened the rehabilitation period while advances in implant design have improved overall clinical results. Patients with successful knee replacements, however, often subjectively feel that even though their knee is pain free that it is still not “normal”. This is in part due to the fact that the anterior cruciate ligament (ACL) is necessarily sacrificed in all complete knee replacements. The result is that the artificial knee does not have the same stability or kinematics through the arc of motion as a normal knee.
Anatomy of the Arthritic Knee
Anatomically the knee is divided into three distinct “compartments”. The arthritic process usually affects all three. The three compartments of the knee include:
- the inside compartment (medial compartment),
- the outside compartment (the lateral compartment)
- the kneecap joint (patellofemoral compartment).
When the arthritic knee becomes painful enough so that surgery is necessary and all three of the knee compartments are involved, conventional full tri-compartmental replacement of all three of these compartments is necessary. This complete knee replacement has become the “gold standard” operative procedure for treatment of the arthritic knee and is far and away the most common type of knee replacement procedure performed. However, arthritis of the knee is sometimes limited to just one of the knee compartments. It is not uncommon for the arthritis to be limited to the medial compartment. In this special circumstance it is possible to replace only the damaged medial or inside part of the knee only instead of the entire joint.
Partial (Hemi) Knee Replacement
In some cases the arthritis is limited to the medial compartment of the knee only. As an alternative to full knee replacement, replacement of the medial compartment of the knee can be performed. This “partial” knee replacement is called the “uni” or “hemi” compartmental knee replacement.
It should be noted that for a variety of reasons, partial knee replacement is limited to the medial compartment. Uni or hemi replacement of the outside or lateral compartment of the knee is rarely recommended or considered even in the presence of isolated lateral compartment disease. Due to variances in anatomy and the weight bearing forces applied, hemi replacements of the lateral compartment tend to fail much more often than those of the medial side of the knee. This is also the case for arthritic disease of patellofemoral compartment. These two specific compartments of the knee are more effectively treated by total knee replacement surgery.
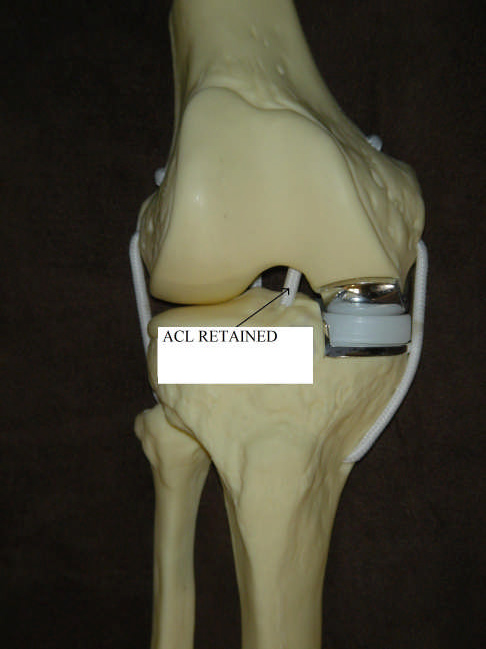 Picture 1. Note that the ACL is retained in the partial knee replacement. It is sacrificed in all complete knee replacements
Picture 1. Note that the ACL is retained in the partial knee replacement. It is sacrificed in all complete knee replacementsOperative Indications and Preop Evaluation
Operative indications for medial compartment hemi knee replacement are as follows:
- Activity and rest pain must be severe enough to justify surgery.
- Patients with mild to moderate pain that can be controlled by other measures such as use of nonsteroidal anti-inflammatants (NSAIDS), steroid (cortisone) injections, viscosupplementation hyaluronate injections (Synvisc, Hyalgan and others), or arthroscopic surgical measures should not be considered for partial arthroplasty.
- The pain should primarily be located over the inside of the knee joint.
- X-rays must demonstrate that the arthritis is primarily limited to the medial compartment of the knee.
- Stress x-rays where the lateral compartment is placed under compressive force can help determine if there is any arthritic lateral joint space narrowing. If present, partial knee replacement can not be considered as a surgical option.
- Occasionally MRI studies of the knee and even diagnostic arthroscopy to directly visualize the interior of the knee may be necessary to determine if a patient is a candidate for partial replacement.
Partial Contraindications
As previously mentioned, coexisting significant lateral compartment arthritic disease is the major contraindication to medial compartment hemi knee replacement. Patellofemoral disease, if not severe, is not an absolute contraindication. However symptoms related to the patellofemoral joint will not be relieved by hemi replacement surgery. Arthritic kneecap symptoms generally include anterior knee pain accentuated by squatting or stair climbing.
Also, the anterior cruciate ligament (ACL) must be intact. A patient with a previous disruption of the ACL is not a candidate for hemi replacement surgery.
Patrial Replacement Unique Risks
Partial knee replacement has been performed in some fashion for nearly three decades. Popularity of the hemi replacement surgery has fluctuated. Historically the primary problems with partial knee replacement surgery have been:
- The risk of early implant loosening
- Wearing away of the plastic polyethylene bearing surface.
Implant Loosening
Cement fixation is the standard method of attaching all knee implants to bone. This is true for both hemi and full replacements. Cemented full knee replacements are predictably successful and relatively durable. The cement bond of full knee replacement implants will typically last 15 years or more before loosening occurs.
Over the last 25 years the results of cemented partial replacements have not been so predictable and durable. Early implant loosening over the first two to three years, particularly of the tibial component, has been noted to sometimes occur. The primary reason for this increased loosening risk appears to be due to the fact that the cemented surface area of the hemi knee to bone is much smaller (less than half) than that of the full replacement. As the forces of weight bearing and activity are distributed over this smaller surface area, the cement bond of the implant to bone can occasionally be overwhelmed and lead to early loosening. Early implant loosening does not occur in every case or in even most cases, but it does occur with enough frequency to make some surgeons hesitant in recommending partial knee replacement as a surgical option. Meanwhile, the quest has been continued to eliminate this risk by finding a method of reducing the stresses on the bone cement interface.
Polyethylene Wear
A second risk unique to partial knee replacements is the potential for accelerated polyethylene “plastic” wear. The plastic polyethylene “cushion” between the femoral and tibial implants of a full replacement typically will wear down to the point of requiring a fairly simple plastic exchange in 10 to 12 years. Historically polyethylene wear occurs at a faster rate in the partial knee. In an effort to protect the bone cement interface and reduce shear forces to which it may be subjected, tibial polyethylene plastic designs are usually made relatively flat. These flat plastic articulations, though probably protective of the cement, have been found to increase the rate of wear of the tibial polyethylene bearing surface over that found with a more curved conforming articulation.
 Picture 2. Fixed bearing hemi knee replacement. The tibial polyethylene is rigidly fixed to the underlying metal base plate. In other fixed bearing knee designs, the poly is cemented directly to the bone without an intervening metal base plate.
Picture 2. Fixed bearing hemi knee replacement. The tibial polyethylene is rigidly fixed to the underlying metal base plate. In other fixed bearing knee designs, the poly is cemented directly to the bone without an intervening metal base plate.Partial Replacement Advantages
There are several potential significant advantages of hemi knee replacement surgery. They include:
- Preservation of healthy and normal compartments of the knee.
- The operation is more amenable to the “minimal incision approach” leading to faster recovery and rehabilitation and a quicker return to full activity.
- Even when unsuccessful, revision to a conventional full replacement is a relatively straight forward surgical procedure with results nearly equaling those of primary full replacement surgery.
- The anterior cruciate ligament (ACL) is preserved in partial replacement. The ACL is routinely sacrificed in all full knee replacement procedures. Sacrifice of the ACL in full knee replacements can lead to the sense of knee being somewhat “lax” or loose by the patient. Operative techniques are employed by the surgeon to minimize the effect of this by skillful methods of intra-operative balancing of the knee ligaments. The ACL deficiency of a full replacement seems more noticeable to some patients than others, but few patients with complete knee replacement sense that their artificial knee feels “normal”. Hemi knee replacement patients, on the other hand, typically find their new joint feels much more like a normal knee due to the preservation of the ACL and of normal knee stability.
The Mobile Bearing Replacement:
A Potential Solution to Partial Problems
Mobile Bearing Knee Design Differences
An implant has been designed to address the potential hemi compartmental knee replacement problems of early implant loosening and accelerated polyethylene wear. This implant is the Oxford Mobile Bearing Partial Knee. Developed by surgeons in Oxford, England almost 20 years ago, it was released by the FDA for use in the United States in April of 2004. The Oxford group has long term clinical data demonstrating the increased durability and dependability of the mobile bearing design.
There are two major differences between the Oxford Knee and other hemi knee replacements. These include:
- The polyethylene articular insert is “mobile”. In other hemi knee designs the plastic bearing surface is fixed rigidly to the underlying metal tibial base (or in the case of an all plastic tibial implant with no metal backing, directly to the bone). When sheer stress is applied to the plastic of these fixed bearing implants it is transferred directly to the bone cement interface. These stresses are believed to accelerate loosening of the cement from the bone. In the Oxford Mobile Bearing Knee the plastic insert is allowed to freely “float” on top of the tibial base. Sheer stresses are absorbed by the mobility of the polyethylene insert thus protecting the underlying bone cement interface. The result is an implant that theoretically should be more resistant to the forces leading to implant loosening.
- Because the polyethylene insert is mobile, it can be designed with a curved articular surface exactly conforming to the curve of the femoral implant in all planes. This matched radius of curvature spreads the weight bearing out over the entire polyethylene surface thus reducing the stress and wear. Extensive studies from England’s Oxford group have confirmed that the wear rate of the poly in the Oxford Mobile Bearing Knee is extremely low. This type of polyethylene conformity can not be utilized in other fixed bearing implant systems because it increases sheer stresses in the bone cement interface leading to potential early loosening, a problem avoided in the Oxford knee by the mobility of its polyethylene insert.
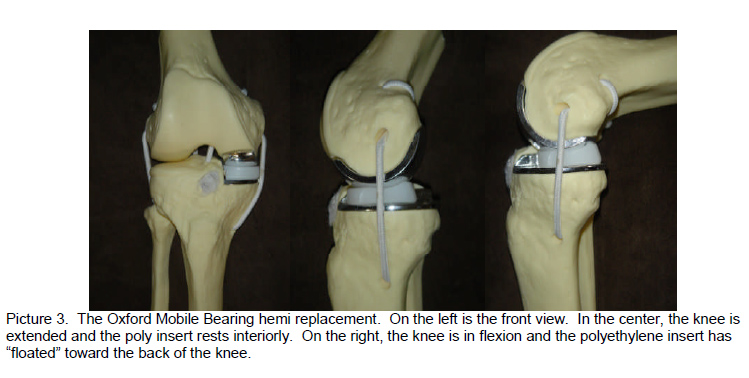
Mobile Bearing Design Results
The Oxford group has reported clear data that demonstrates the successfulness of the mobile bearing design concept. The problem of poly (plastic) wear seems to largely be eliminated. The demonstrated wear rate is extremely slow. The problem of loosening has similarly found to be minimized or nearly eliminated through the first decade of follow up. The Oxford group reports that over 95% of their implants survive the first decade. Other European surgeons have reported results in line with the findings noted by the Oxford group.
However, as mentioned, the implant has been available to U.S. surgeons for routine implantation only since April 2004. And until we have long term follow up using strict standards of evaluation in this country there will be some wariness regarding these European results. Not all seemingly good European ideas have in the past stood the test of strict scientific American scrutiny over time.
Conclusion
The partial (hemi) knee replacement is an inherently appealing option for the treatment of isolated medial compartment arthritis of the knee. As opposed to the full tricompartmental knee replacement, the hemi replacement preserves the anterior cruciate ligament. The result is the maintenance of normal knee stability leading to a joint that feels more “normal”. The hemi knee replacement is more amenable to minimal incision surgical techniques thus shortening the hospital stay and the rehab and recovery period. Compartments of the knee unaffected by the arthritic process are preserved.
Historically the risks of conventional uni replacements have included a greater risk of early implant loosening and of the possibility of accelerated polyethylene (plastic) wear. The Oxford Mobile Bearing Partial Replacement addresses these risks by its unique design features. European data thus far demonstrates the successfulness of the mobile bearing design. Further follow up in this country is needed to confirm this. However, the mobile bearing design of the Oxford Knee does physiologically make sense and hopefully will become the surgical procedure of choice for patients with isolated medial compartment arthritis of the knee.



 Our patients can receive MRI imaging onsite at both our Louisville and New Albany Clinics.
Our patients can receive MRI imaging onsite at both our Louisville and New Albany Clinics. Providing the latest advances in orthopedic surgery is our specialty.
Providing the latest advances in orthopedic surgery is our specialty. We take a unique, multidisciplinary approach to pain management.
We take a unique, multidisciplinary approach to pain management. Our physical therapists use advanced techniques to help restore strength and mobility.
Our physical therapists use advanced techniques to help restore strength and mobility.  We provide comprehensive, conservative care for a wide variety of foot and ankle conditions.
We provide comprehensive, conservative care for a wide variety of foot and ankle conditions. We offer same- and next-day care to patients with acute injuries.
We offer same- and next-day care to patients with acute injuries. Get back in the game with help from our sports medicine specialists.
Get back in the game with help from our sports medicine specialists.  Our centers are equipped with a state-of-the-art digital X-ray machine.
Our centers are equipped with a state-of-the-art digital X-ray machine.